Cutaneous Wound Closure Materials: Focus on Surgical Zippers
Introduction
Dermasurgeons frequently treat a broad range of wounds that need to be closed effectively. While staples and sutures are still the most common traditional techniques, surgical zippers offer a promising non-invasive, customizable, and patient-friendly substitute. In clinical practice, choosing a closure method that strikes a compromise between robust wound support, aesthetic results, affordability, and usability is essential. In order to give doctors an evidence-based guide, this study examines the evolution, clinical uses, and relative efficacy of surgical zippers in comparison to other closure materials.
Materials and Methods
An independent, comprehensive literature search was conducted using PubMed, Cochrane Library, Google Scholar, and Ovid. The focus was on English-language articles from 1990 onwards addressing skin closure materials including sutures, staples, adhesive tapes, tissue adhesives, and surgical zippers. Clinical studies, reviews, and case reports were included to evaluate safety,
efficacy, and practical considerations.
Tissue Adhesives
Tissue adhesives, particularly those based on cyanoacrylate, such as Octyl-2-cyanoacrylate (OCA), have revolutionized skin closure because to their rapid polymerization, high tensile strength, and superior cosmetic results. High-viscosity OCA is one example of an advanced formulation that improves wound approximation and decreases adhesive migration. Within 5–10 days after application, these adhesives peel off spontaneously as the epithelium re-epithelializes. Benefits include a decreased risk of infection, a shorter recovery period, no needlestick injuries, and appropriateness for young patients. OCA has antibacterial qualities as well. Cons: More expensive, more sensitive to application method, and not suitable for high-tension, bleeding, or infected wounds.
Adhesive Tapes
Surgical adhesive tapes, which offer suture-less closure, are frequently used to maintain wounds following the removal of staples or sutures or in conjunction with buried dermal stitches in low-tension wounds. They are made to be vapor permeable, water-resistant, and non-allergic. Benefits include decreased infection rates, quicker restoration of tensile strength, cost effectiveness, and decreased local tension. Drawbacks include the possibility of early detachment, inconsistent adherence based on application technique, and restrictions on accurate skin edge estimation.
Absorbable Sutures
Absorbable sutures minimize tissue reactivity and eliminate the need for removal because they break down predictably over a period of about 60 days. They are perfect for tissue beneath the skin. Typical resources consist of: • Natural: Catgut, or surgical gut Polyglycolic acid, polyglactin 910 (Vicryl), polydioxanone, and polyglecaprone 25 (Monocryl) are synthetic ingredients. The fast degradation of Vicryl Rapide, a gamma-irradiated polyglactin 910, which loses 50% of its tensile strength by day 5 and absorbs completely by day 42, makes it useful for temporary wound support and lessens the need for suture removal.
Non-Absorbable Sutures
These sutures offer long-lasting support but must be removed since they are resistant to enzymatic degradation. Silk, nylon, polypropylene, and surgical steel are examples of common materials. For a lower risk of infection, monofilament synthetic sutures are recommended. While some studies favor absorbable sutures for patient comfort and convenience, non-absorbable sutures also exhibit comparable cosmetic and infection outcomes.
Staplers
With the help of disposable mechanical skin staplers, lengthy incisions can be closed up to four times faster. In contrast to metal staples, the Insorb™ dermal stapler uses absorbable U-shaped staples positioned subcutaneously to provide quicker closure, better esthetic results, and reduced infection rates.
Surgical Zipper
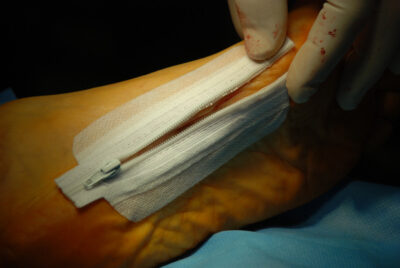
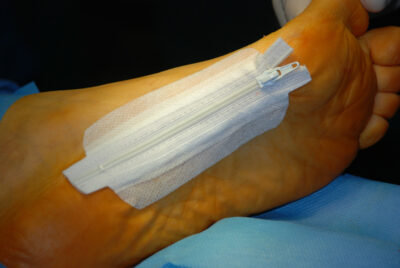
A surgical zipper A non-invasive skin closure method that allows insepection without affecting the closure. It enhances patient comfort, cuts down on operating time, and eliminates the need for removal. It is not appropriate for patients who are obese or have moist, curved, or high-tension wounds. It is particularly helpful for pediatric and oncology patients, as clinical studies demonstrate similar cosmetic and complication outcomes to sutures.
Surgical Zippers’ Mode of Action and Application Process
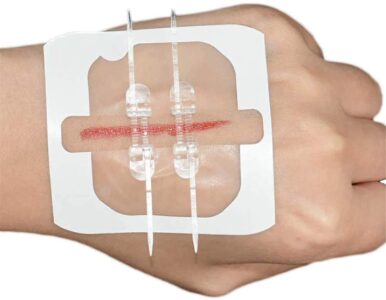
Surgical zippers combine mechanical interlocking and adhesive bonding to provide a non-invasive skin closing method. Like a traditional zipper, the gadget usually comprises of two flexible adhesive strips with interlocking plastic tracks inserted in each. The tracks ensure tension-free closure and maximum healing by precisely aligning the wound edges when they are zipped together.
Mechanism of action
The mechanism relies on two key principles:
1.Adhesive Anchoring: The device is anchored to the skin on each side of the incision by the medical-grade adhesive on each strip. Because of their hypoallergenic, breathable, and water-resistant properties, these adhesives provide dependable adhesion without irritating skin.
- Zipper Interlock: The wound edges can be mechanically joined thanks to the center zipper component. The interlocking teeth minimize stress and lower the risk of infection by softly approximating the skin without puncturing it when the slider is pulled along the tracks.
Surgical zippers preserve epidermal continuity, in contrast to sutures or staples, which pierce the skin and may damage adjacent tissue. Because of this, they are very helpful in minimizing scarring and postoperative discomfort.

Application procedure
- Wound Preparation: Make sure the surrounding skin is dry and clean. The skin should be free of oils and antiseptic residues, and hemostasis should be reached.
- Positioning: Align the adhesive strips parallel to the wound margins, often 0.5–1 cm distant from the incision line. The zipper should sit directly over the middle of the wound.
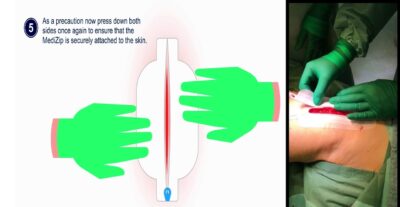
- Adhesive Attachment: To guarantee complete
contact and strong adherence, carefully apply each adhesive strip to the skin, pressing down firmly.
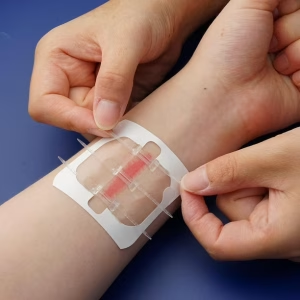
- Closure: Draw the coiled edges into close proximity by zipping the tracks together from one end to the other using the built-in slider or pull tab.
- Inspection and Dressing: Verify that the tension and alignment are correct. If necessary, a sterile dressing may then be applied to the area.
Removal
Gently unzip the device in the opposite way to remove the surgical zipper. After that, the adhesive strips can be gently pulled off the skin.
Laser Tissue Bonding (LTB)
LTB, uses lasers with wavelength-specific dye absorbers (such indocyanine green) and proteinaceous solders (albumin) to accomplish fast tissue bonding without the need for sutures.
Minimal tissue handling, early re-epithelialization, watertight closure, and less scarring are among the benefits. The cost of the equipment, the possibility of thermal harm, and the limited of human trials are the drawbacks, though.
Conclusion
Wound closure choice depends on wound characteristics, patient factors, available materials, and surgeon expertise. Surgical zippers offer a promising non-invasive alternative with advantages in comfort and cosmesis. Absorbable sutures like Vicryl Rapide suit short-term needs, while tissue adhesives provide needle-free closure in appropriate cases. Staplers and laser bonding techniques offer further options tailored to clinical scenarios. An evidence-based approach helps optimize wound healing and patient outcomes.
