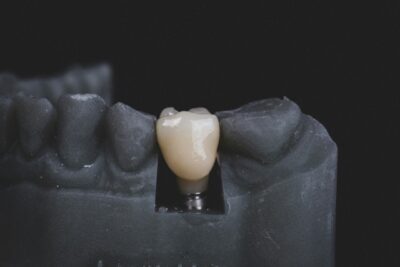
Dental Implants: Your Permanent Solution for Missing Teeth


Are you missing one or more teeth? Dental implants offer a state-of-the-art, long-lasting solution to restore your smile, improve your oral health, and boost your confidence. Since their introduction in the 1960s, dental implants have become the gold standard for tooth replacement, surpassing traditional removable dentures in terms of function, aesthetics, and durability. Whether you’re missing a single tooth, several teeth, or require a full arch restoration, dental implants provide a stable and natural-feeling alternative.
What Exactly Are Dental Implants Made Of?
The core of most dental implants is titanium, a remarkable biocompatible metal. This means your body readily accepts titanium, allowing it to fuse directly with your jawbone in a crucial process called osseointegration. This integration creates an incredibly strong and stable foundation, much like the root of a natural tooth.
Beyond titanium, zirconia implants have emerged as a cutting-edge, metal-free option. Zirconia boasts similar strength and impressive bone-bonding capabilities to titanium, with the added advantage of being tooth-colored. This makes zirconia implants an excellent choice for patients seeking a highly aesthetic outcome, especially in visible areas of the mouth. Clinical studies consistently demonstrate that zirconia implants are just as effective and reliable as their titanium counterparts.
Why Are Dental Implants the Preferred Choice?
Decades of extensive clinical research and real-world experience consistently affirm that dental implants are a safe, highly durable, and aesthetically superior solution for tooth loss. Choosing dental implants offers a myriad of benefits:
- Restored Natural Function and Appearance: Implants look, feel, and function just like your natural teeth, allowing you to eat, speak, and smile with complete confidence.
- Improved Oral Health: Unlike bridges that require altering adjacent healthy teeth, implants stand alone, preserving your natural tooth structure. They also help prevent bone loss in the jaw, which commonly occurs after tooth extraction.
- Preservation of Jawbone: When a tooth is lost, the underlying jawbone can begin to deteriorate. Dental implants stimulate the bone, preventing this loss and maintaining the natural contours of your face.
- Long-Term Durability: With proper care, dental implants can last a lifetime, making them a wise investment in your oral health and overall well-being.
However, it’s crucial to remember that just like natural teeth, implants require diligent care. Maintaining excellent oral hygiene through regular brushing and flossing, coupled with routine dental checkups, is essential to prevent peri-implant diseases. These conditions, if left unchecked, can lead to inflammation, bone loss around the implant, and ultimately, implant failure. Your commitment to good oral care is paramount to the long-term success of your dental implants.
Understanding the Components of a Dental Implant
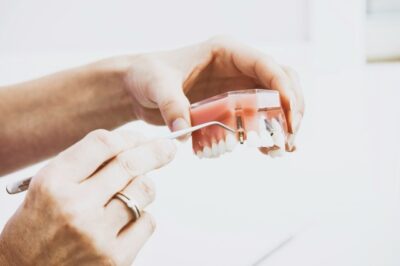
A typical dental implant system is comprised of three distinct, yet interconnected, parts working in harmony to mimic a natural tooth:
- The Implant (Fixture): This is the screw-shaped titanium or zirconia post (ranging from 4–16 mm in length) that is surgically placed into your jawbone. It serves as the artificial tooth root, providing the foundational stability for your new tooth.
- The Abutment: A small connector piece that screws into the top of the implant after it has successfully integrated with the bone. The abutment extends through the gum line and acts as the support structure for your final prosthetic.
- The Crown/Bridge/Denture: This is the visible part of your tooth replacement, custom-designed to perfectly match the color, shape, and size of your natural teeth. It can be an individual crown for a single missing tooth, a bridge for multiple missing teeth, or even secure a full denture for a more stable and comfortable fit.
It’s worth noting that some modern implant systems feature a one-piece design, where the abutment is integrated directly with the implant body, streamlining the treatment process in certain cases.
Osseointegration: The Vital Healing Process
Following implant placement, a critical biological process called osseointegration begins. This is where your jawbone cells grow directly onto and fuse with the surface of the implant, creating an incredibly strong and stable anchor. This healing period typically takes 2 to 6 months, depending on individual healing capabilities and bone quality. Once osseointegration is complete, the implant is strong enough to reliably support the permanent restoration.
Advancements in dental implantology have also introduced innovative techniques:
- Immediate Implant Placement: In favorable situations, an implant can be placed into the tooth socket immediately after a tooth extraction, potentially reducing the overall treatment time.
- Immediate Loading: If the implant achieves exceptional initial stability during placement, a temporary crown or restoration can sometimes be attached on the very same day. This allows patients to have a visible tooth replacement much sooner.
Always consult with your dentist or periodontist to determine if you are a suitable candidate for these advanced and time-saving techniques.
The Stages of Your Dental Implant Journey

The process of getting dental implants is a meticulously planned and executed journey, typically involving several key stages:
-
Comprehensive Examination & Personalized Planning:
Your journey begins with a thorough consultation with your dentist or periodontist. This crucial initial phase involves:
-
- A detailed clinical oral examination of your teeth, gums, and overall oral health.
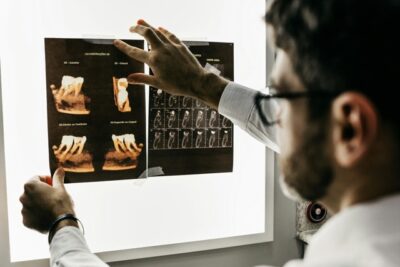
- Advanced imaging, including digital X-rays and often a Cone Beam Computed Tomography (CBCT) scan. CBCT scans provide highly detailed 3D images of your jawbone, allowing your dentist to precisely assess bone quality and quantity, and to accurately locate vital structures like nerves and sinuses, ensuring a safe and predictable surgical outcome.
- 3D planning and virtual surgery may be utilized, especially if bone grafting or other bone reconstruction procedures are anticipated, allowing for precise implant positioning.
- Precise Implant Placement Surgery:
Implant surgery can follow one of two primary protocols:
-
- One-stage Protocol: In this approach, the dental implant and a small healing cap are placed in a single surgical procedure. The healing cap remains visible above the gum line throughout the osseointegration period. Once healing is complete, the healing cap is removed, and the final abutment and crown are attached.
- Two-stage Protocol: This method is often recommended for more complex cases or when bone grafting is performed. A cover screw is placed on the implant, and the gum tissue is stitched closed over it, completely concealing the implant during the healing phase. After successful osseointegration, a second, minor surgical procedure is performed to gently expose the implant and attach the abutment.
Your dental professional will determine the most appropriate surgical protocol based on your unique clinical situation.
-
Tooth Preparation & Impression Taking:
Once the osseointegration process is complete and the implant is firmly integrated with your bone, your dentist will take highly accurate impressions of your teeth and the implant. These impressions, often digital scans, are then sent to a specialized dental laboratory. Here, skilled dental technicians meticulously design and fabricate your custom crown, bridge, or denture, ensuring it blends seamlessly with your natural smile in terms of shape, size, and color.
-
Fitting the Final Restoration & Post-Care:
In the final stage, your custom-designed crown, bridge, or denture is carefully cemented or screwed onto the implant abutment. Your dentist will meticulously check for proper fit, ensure your bite alignment is comfortable and functional, and make any necessary adjustments for optimal comfort and aesthetics. Regular follow-up visits will be scheduled to monitor the performance of your implants and ensure their long-term success.
Bone Grafting & Guided Bone Regeneration (GBR): Building a Strong Foundation
In some instances, the jawbone may have insufficient height, width, or density to adequately support dental implants. This can occur due to long-term tooth loss, periodontal disease, trauma, or certain medical conditions. In such cases, bone grafting or guided bone regeneration (GBR) procedures are essential to create a robust foundation for successful implant placement.
Common Types of Bone Grafts:
- Autografts: Considered the “gold standard,” autografts involve harvesting bone tissue from another site within your own body (e.g., your hip, chin, or tibia). Autografts offer the best biological compatibility and eliminate the risk of rejection.
- Allografts: These are bone grafts derived from donated human bone, meticulously processed and sterilized by a bone bank.
- Xenografts: Bone material sourced from animal species, most commonly bovine (cow) bone, which is carefully processed to be safe for human use.
- Alloplasts: Synthetic, biocompatible bone-like materials, often made from calcium phosphate compounds, which can stimulate new bone growth.
After a bone grafting procedure, a healing period of at least three to six months is typically required to allow the grafted bone to mature and integrate before implant placement can proceed.
Guided Bone Regeneration (GBR)
GBR is a specialized technique that involves placing a barrier membrane over a bone defect or a bone graft. This membrane serves a crucial purpose: it prevents faster-growing soft tissue cells (like gum cells) from migrating into the bone defect, thereby creating and protecting the space necessary for slower-growing bone cells to regenerate the lost bone tissue.
Membranes used in GBR can be:
- Resorbable: These membranes naturally dissolve and are absorbed by the body over time, eliminating the need for a second surgical procedure for removal.
- Non-resorbable: These membranes are made from materials that do not dissolve and therefore require a second, minor surgical procedure for their removal after the bone has healed.
Conclusion: Invest in Your Smile, Invest in Yourself
Dental implants represent a monumental leap forward in restorative dentistry, offering a reliable, long-lasting, and aesthetically superior solution for tooth replacement. With meticulous planning, advanced modern techniques, and your commitment to diligent oral hygiene and regular dental checkups, dental implants can profoundly restore your smile, chewing function, and overall confidence for decades to come. Don’t let missing teeth hold you back – explore the transformative possibilities of dental implants and rediscover the joy of a complete and healthy smile.